You Inspire The Best in Us.
With the many advances in care and treatments, today’s patients have more and more reasons to expect the best outcomes. Here are the incredible stories of our patients and their journeys. Click on a thumbnail and scroll down to view each story.

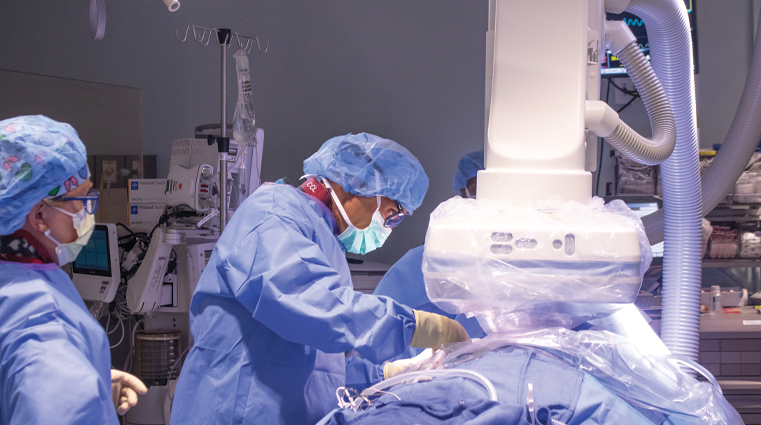
The Electrical Activity of the McLeod Health Electrophysiology Program
By Ashley Boles & Tammy White
McLeod Health Electrophysiologists bring a diverse blend of skill and expertise – including designing part of the Playstation 3, Xbox and supercomputers – to the patients they serve.
Dr. Prabal Guha and Dr. Cyrus Kocherla at McLeod Regional Medical Center and Dr. Yuxuan Mao at McLeod Health Seacoast are Electrophysiologists who specialize in evaluating the abnormalities of the heart’s rhythm. Their focus is on the heart’s electrical system and how it impacts overall cardiac function.
McLeod offers a broad range of advanced electrophysiology services, including leadless pacemakers, defibrillators, internal loop recorders, ablations with 3D mapping, and the left atrial appendage closure device (also known as the Watchman™ Implant).
Two newer offerings further expand treatment options: cardiac contractility modulation (CCM) and the concomitant procedure.
Electrophysiology plays a critical role in diagnosing and treating atrial fibrillation, a heart condition in which the heart’s upper chamber beats irregularly.
Initial treatment may include medication or an electrical shock to the heart to restore heart rhythm. When these methods are unsuccessful, an ablation may be performed. This catheter-based procedure reroutes abnormal electrical signals in the heart.
At McLeod Health, Drs. Guha, Kocherla and Mao perform ablations using the FDA-approved pulsed field ablation (PFA). This procedure uses brief electrical pulses to treat abnormal rhythms while minimizing impact on surrounding tissue.
Atrial fibrillation can also cause blood to pool in the left atrial appendage, an area of the heart where clots commonly form. These clots may travel to the brain and cause a stroke. To reduce this risk, McLeod offers the left atrial appendage closure (LAAC) device, which is implanted at the opening of the left atrial appendage to prevent blood clots from entering the blood stream.
For patients who need both an atrial fibrillation ablation and the LAAC device, McLeod now offers a combined approach known as a concomitant procedure.
This single procedure addresses both the abnormalheart rhythm and the associated stroke risk.
“Traditionally, these were performed as standalone procedures,” said Dr. Kocherla. “Combining them is a greater convenience for our patients. It can improve recovery, reduce the hospital stay and shorten the need for blood thinners postoperatively.
“It is safe to have both procedures performed at the same time, and the data shows no increase in complication rates.
“Our patients appreciate having everything completed in one visit,” added Dr. Kocherla.
Another advanced option available at McLeod is cardiac contractility modulation, a therapy designed for patients with heart failure who have not responded adequately to medication. This small implantable device improves the heart’s ability to contract, helping reduce heart failure symptoms and improve quality of life.
“Cardiac contractility is a measure of the strength of the cardiac muscle,” said Dr. Guha. “To properly pump enough blood throughout the body, the heart’s muscle must reach a certain level of force. Heart failure negatively impacts that strength.”
Standard treatment for heart failure begins with medication. When medications alone are not effective, patients may be candidates for the CCM device.
“The CCM device looks like a pacemaker,” said Dr. Guha. “Through a small incision in the chest, the device is implanted beneath the skin and connected to leads placed in the heart muscle. These leads deliver a strong electrical pulse several times a day to help the heart contract.”
While heart failure cannot be cured, it can be managed. CCM can help patients perform everyday activities more comfortably, such as walking short distances or climbing stairs, with less fatigue.
Dr. Yuxuan Mao joined the Electrophysiology team at McLeod Health Seacoast in August 2025.
Dr. Mao didn’t have a typical introduction to medicine. After earning his undergraduate degree, he spent several years working for IBM in Raleigh, North Carolina.
“I had the good fortune to work on some amazing projects like designing part of the PlayStation 3, Xbox, and supercomputers. But I felt something was missing and wanted a more meaningful vocation. I found that in medicine. Electrophysiology allows me to use my engineering know-how to serve patients in need and allows me to utilize the latest technology to potentially cure someone's disease,” said Dr. Mao.
Dr. Mao performs radiofrequency and pulsed field ablations for patients with atrial fibrillation, supraventricular tachycardia (SVT), and premature ventricular contractions (PVC). He also works with patients with atrial fibrillation who take blood thinners but experience bleeding complications, offering implant-based solutions that may allow them to discontinue those medications.
“I love coming to work every day because we all share the same mission – to make a positive difference in our patients’ lives, and provide much needed access to Electrophysiology care,” said Dr. Mao. “I look forward to bringing the latest and most advanced treatment techniques to the people of Horry County and beyond.”
-
McLEOD REGIONAL MEDICAL CENTER FLORENCE
843-777-2000 -
McLEOD DARLINGTON
843-777-1100 -
McLEOD DILLON
843-774-4111 -
McLEOD LORIS
843-716-7000 -
McLEOD SEACOAST
843-390-8100 -
McLEOD CHERAW
843-537-7881 -
McLEOD CLARENDON
803-433-3000



-
McLEOD REGIONAL MEDICAL CENTER FLORENCE
843-777-2000 -
McLEOD DARLINGTON
843-777-1100 -
McLEOD DILLON
843-774-4111 -
McLEOD LORIS
843-716-7000 -
McLEOD SEACOAST
843-390-8100 -
McLEOD CHERAW
843-537-7881 -
McLEOD CLARENDON
803-433-3000
 Find a Doctor
Find a Doctor  Locations
Locations  Services
Services