Stories


Child Life Services Expand to Serve All Pediatric Patients
NASCAR Foundation Joins Donors to Further Support McLeod
Harsh lights, beeping equipment, caregivers bustling in and out -- hospitalization is stressful for most adults. But imagine this from a young child’s perspective: sick, in pain, and removed from everything familiar. However, thanks to generous gifts to the McLeod Health Foundation, the McLeod Children’s Hospital Child Life Program has been making hospital stays easier, more kid-friendly, and even surprisingly fun at times.
Cory Prescott, McLeod’s Child Life Coordinator, guides and reassures patients and their families in the Pediatric Intensive Care Unit and on the Pediatric Floor. “Positivity is our goal,” Cory says. “Providing a comfortable and stress-free space makes their stay feel less like a hospital and more like a hotel with fun toys and activities.”
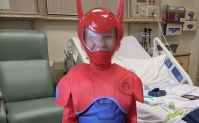
Maggie Bellflowers experienced the ongoing evolution of the Child Life Activity Center when her son Owen, a kindergartener at the time, was hospitalized with three highly contagious viruses.
“The playroom was like being in the Hilton,” Maggie remembers. “His eyes grew three sizes when he saw it. He gasped, ‘Mama, I want to go there!’”
Although in isolation in his own room, Cory and her staff brought the Child Life Activity Center to Owen.
“He felt so much love and compassion,” Maggie continued, “Owen got to choose the toys he wanted to play with: a teddy bear, coloring books, a comfortable blanket, and his favorite: a Spider Man playset to keep. I was blown away and said, ‘Do you spoil every patient like this? Cory smiled and said, “Yes. Yes, we do.’”
What started out as overwhelming became calm. “My anxiety about my young child melted away,” Maggie said. “It was such a relief to hear him say, ‘Mama, I don’t need you. I’m fine here with the nurses.’”
Even when it was time to remove his IV port, which Owen was apprehensive about, Cory calmed his fears.
“A child’s experience with the medical world sets the tone for how they view and use healthcare services for the rest of their lives,” says Cory. “Our donors help us transform the idea of what a hospital can be.”
And today the treasured Spiderman playset is still in Owen’s bedroom at home.
NASCAR Foundation Provides Grant for Child Life Activity Center in the McLeod Day Hospital
The NASCAR Foundation is a shining example of how donors further assist pediatric patients at McLeod. They recently provided a grant to create a separate Child Life Activity Center in the McLeod Day Hospital for outpatient pediatric surgery patients. The center provides an environment where children can engage in fun activities prior to surgery, reducing anxiety for both the child and family.
“This grant has transformed a somewhat sterile playroom into a fun and joyful one,” Cory added.
-
McLEOD REGIONAL MEDICAL CENTER FLORENCE
843-777-2000 -
McLEOD DARLINGTON
843-777-1100 -
McLEOD DILLON
843-774-4111 -
McLEOD LORIS
843-716-7000 -
McLEOD SEACOAST
843-390-8100 -
McLEOD CHERAW
843-537-7881 -
McLEOD CLARENDON
803-433-3000


McLEOD HEALTH FOUNDATION